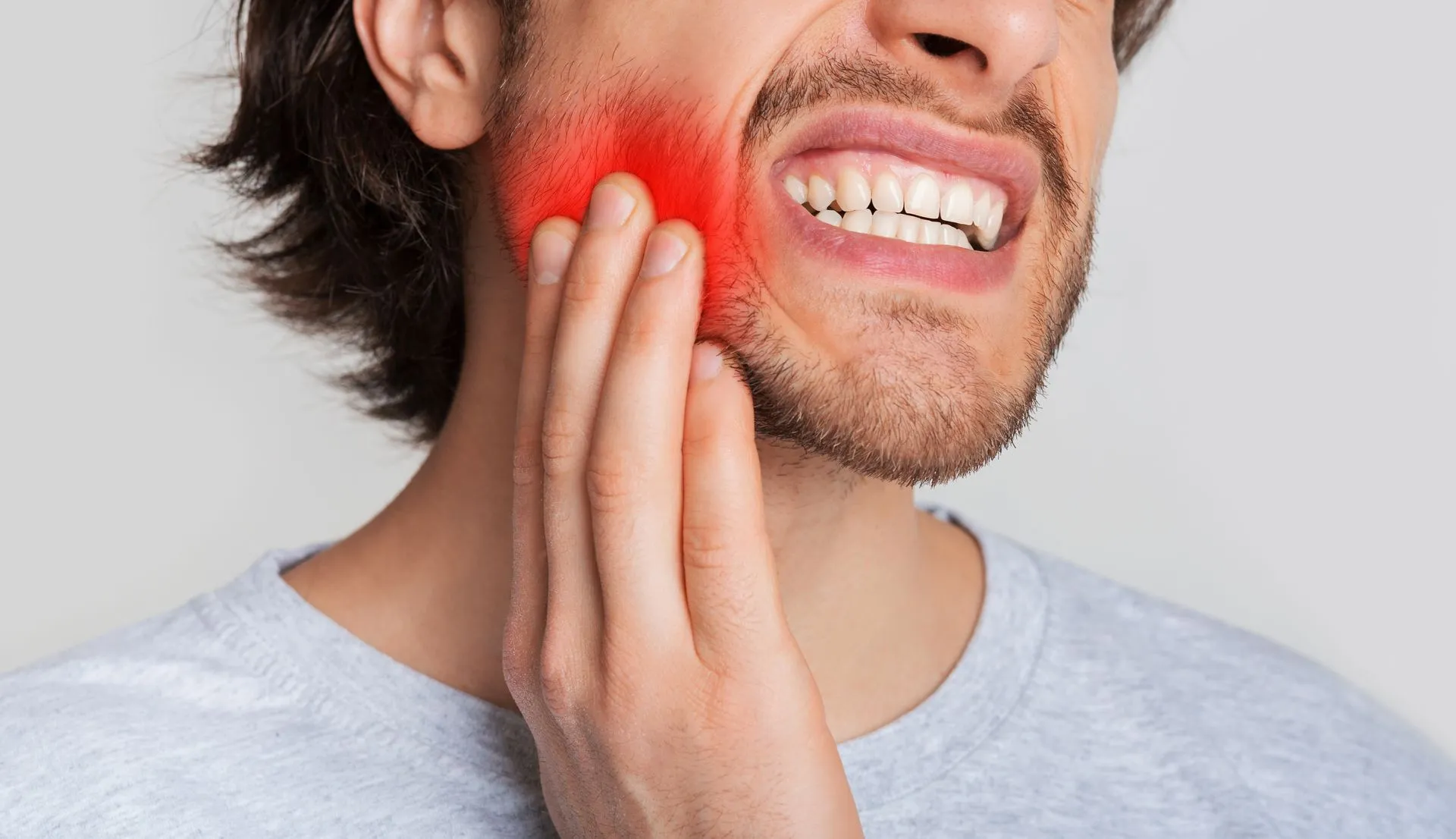
It is indeed an unpleasant pain that can cause limitations in opening the mouth, speaking, eating, and other social skills.
Note that this discomfort is not always associated with the teeth and gums and can also arise as a consequence of infections and/or inflammation in the ears, joints, and salivary glands, among others.
Although jaw pain may disappear spontaneously, one should not ignore the problem, as its occurrence can be cyclical and require differentiated medical treatment.
What is the jaw/maxilla?
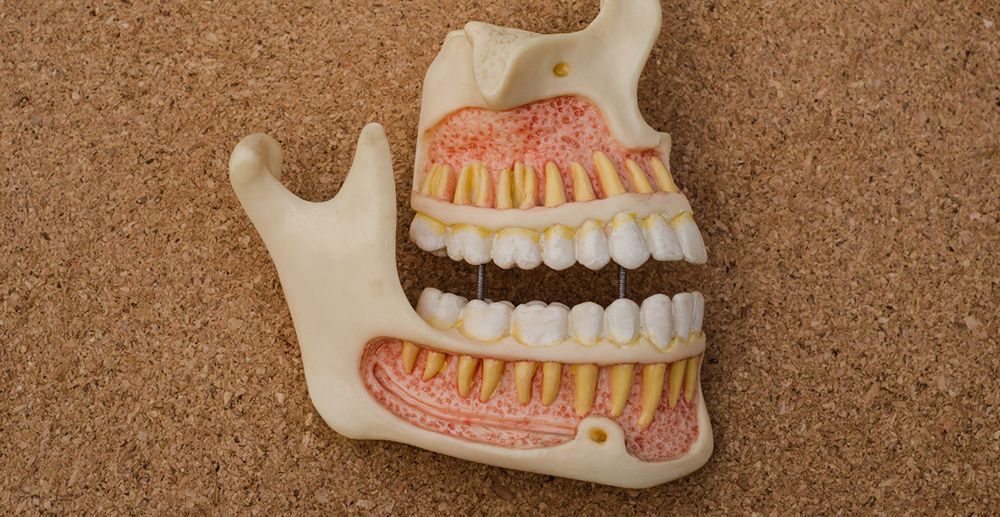
The mandible or lower jaw and the upper maxilla are integral parts of our facial anatomy.
The maxilla or upper jaw is immobile and houses the upper dental arch, while the mandible or lower jaw, which is movable and connected to the skull via the temporomandibular joint (TMJ), houses the lower dental arch. Together with muscles and ligaments, these bones are essential for enabling our eating, phonetics, facial expression, and many other social skills.
Causes of jaw pain
1) Bruxism
Bruxism is a disorder characterized by the involuntary and repeated contraction of the chewing muscles, resulting in the clenching or grinding of teeth. The force generated by these muscles exceeds the physiological tolerance limit, potentially leading to inflammation and structural damage to the muscles and various structures of the temporomandibular joint (TMJ). There is also the possibility of causing premature and excessive wear of the teeth. These phenomena can lead to dental fractures, tooth sensitivity, pain during mouth opening and closing while chewing and speaking, and even headaches.
This phenomenon is certainly one of the main culprits for jaw pain.
2) Temporomandibular Joint (TMJ) Dysfunction
Temporomandibular Joint (TMJ) Dysfunction is defined as a set of disorders involving the masticatory muscles and structures of the temporomandibular joint (articular disc, ligaments, articular capsule). They may arise as a consequence of trauma, bruxism, degenerative changes, etc. Pain and clicking in the jaw/ear, discomfort in the face, and limited movement of the mouth opening and closing are very common in this clinical picture and can vary in intensity and duration.
3) Oro-facial pain of neurovascular origin
There is a set of pathologies, whose diagnosis is not always easy, that arise from alterations in the nerve or vascular branches of the orofacial region, either due to trauma or other causes, leading to headaches, shock-like pain, and cluster headaches. They can be short-lived and stabbing, or of more moderate intensity and long duration. In some clinical scenarios, such as trigeminal neuralgia, there is a strong impact on patients' daily lives. Talking, laughing, washing the face and teeth, and any common stimuli in the facial region become quite painful tasks.
4) Dental Caries
Dental caries is the most common disease of the oral cavity, affecting almost 90% of the world population (WHO) and impacting people of all age groups. Diets high in sugar and lack of oral hygiene are the main causes of the development of caries. Dental caries is characterized by the demineralization of teeth with subsequent softening and development of cavities. They usually have an initial asymptomatic evolution.
Over time, the cavities become deeper, potentially leading to spontaneous pain or pain in response to stimuli such as hot, cold, sweet, or chewing. These pains can be intense and associated with the formation of abscesses, requiring urgent dental treatment.
Regular visits to the dentist/oral hygienist allow for timely diagnosis of these lesions.
5) Wisdom Teeth
Wisdom teeth are the last permanent teeth to erupt, and there is generally not enough space in the jaws to accommodate them. During the eruption of a wisdom tooth, a pericoronitis may develop, which is a severe inflammation and/or infection of the soft tissues surrounding it, sometimes causing intense pain that requires medication and/or tooth extraction.
6) Periodontal Disease
In periodontitis and/or gingivitis, due to the action of bacteria present in dental plaque, there is an inflammation of the gums, sometimes intense, with increased volume of the gums, a more reddish coloration, bleeding, and gum recession. Although less frequent, this condition can also cause jaw pain.
7) Sinusitis
Sinusitis is inflammation and/or infection of the paranasal and maxillary sinuses, which are hollow cavities located in some facial bones and communicate with each other. They can cause symptoms similar to pain in the upper jaw, congestion, and headaches.
8) Oral Cancer
Oral cancer is a collection of malignant tumors that affect the oral cavity (lips, tongue, floor of the mouth, palate, buccal mucosa, salivary glands, pharynx, and jaw bones). It is the 6th most common cancer associated with high mortality rates. It may manifest as persistent ulcers, wounds that do not heal, sudden dental mobility, pain, changes/loss of sensitivity, difficulties in swallowing, and swelling.
Early diagnosis is essential for successful treatment; therefore, visiting the dentist twice a year is of utmost importance.
9) Mumps
Mumps is a viral infection of the parotid salivary glands, located near the branch of the mandible, below each ear. It causes swelling in these glands, potentially triggering pain when chewing and swallowing. As a viral infection, antibiotics are not useful for treatment; emphasis should be placed on antipyretic medication in case of fever, increased water intake, and moist heat in the area. It primarily affects young adults who were not vaccinated against mumps as children.
How to relieve jaw tension?
There are some tricks you can do to relieve jaw tension, such as:
Yoga and meditation (reduce stress).
Avoid eating tougher and elastic foods (chewing gum, bread, candies).
Medications under medical supervision (anti-inflammatories and muscle relaxants).
Moist heat.
Massage the chewing muscles and perform relaxation exercises for them.
Improve sleep.
Remember that, although it can alleviate jaw pain, effective treatment depends on an accurate diagnosis. It is therefore essential to schedule an appointment with the dentist so that together they can determine the most suitable treatment for jaw pain.

Treatment
Pain in the jaw is very common and can arise for various reasons throughout our lives. It is indeed an unpleasant pain that can cause limitations in opening the mouth, speaking, eating, and other social skills. Note that this discomfort is not always associated with teeth and gums and can also arise as a consequence of infections and/or inflammations in the ears, joints, and salivary glands among others.
Although jaw pain can disappear spontaneously, the problem should not be ignored, as its appearance can be cyclical and require differentiated medical treatment.
Botox® Injections
Botox® (botulinum toxin) is injected into muscles with high hyperactivity that cause headaches, joint pain, dental wear, and limitations in mouth movements. The injection will decrease muscle contraction and thus control the referred symptoms caused by jaw pain and reduce the consequences for the temporomandibular joint and teeth.
Myorelaxant Splint
If you suffer from bruxism, a splint may be prescribed for you to use during sleep. Since, unlike the waking state, we do not have voluntary control over the chewing muscles during sleep, the splint will help promote relaxation and, by being placed between the upper and lower jaw teeth, protect them from wear and fracture. Muscle relaxation will also decrease the load on the joint and thus reduce muscle and joint pain, improving comfort in functional movements.
Medication
As an adjunct to other treatment strategies, medication such as anti-inflammatories, muscle relaxants, anxiolytics, and antidepressants can help control the clinical picture. By improving sleep quality, decreasing muscle contraction, and the inflammatory mediators present in the joint and overactive muscles, medication can be very effective in controlling jaw pain. Speak first with a specialized doctor so that the therapy is adjusted to your particular case.
Orofacial Physiotherapy
Orofacial Physiotherapy is a very beneficial tool in the treatment and control of temporomandibular dysfunction. After a thorough diagnosis that includes the temporomandibular joint, the facial and head muscles, and the cervical spine, exercises and movements are carried out and prescribed to strengthen, stretch, and relax the chewing muscles as well as to increase joint mobility.
ATM Viscosupplementation
It consists of injecting hyaluronic acid into the temporomandibular joint. This substance will promote washing, hydration, and lubrication of the joint, thus improving its biomechanics and potentially reducing signs and symptoms such as jaw pain, clicks, and crepitations.
TMJ Surgery (temporomandibular joint)
Different surgical approaches such as arthrocentesis and arthroscopy may be considered in the treatment of temporomandibular dysfunction. These therapies are reserved for severe cases in which patients' signs and symptoms are so painful, prolonged, and debilitating that they prevent the performance of their daily routine such as eating, speaking, or swallowing.
Remember, jaw pain should not be underestimated and the later the diagnosis, the more difficult treatment will be. If you experience any of these symptoms, MALO CLINIC provides an evaluation consultation, where you can have the opportunity to understand your problem and identify treatment possibilities.